If there is a strong inhusion between the retina and the vitreous, the posterior vitreous detachment can cause a traction on the retina.
If the retina itself is fragile at the particular point this can lead to a retinal tear, which will allow the intraoccular fluids to go through and detach the retina.
In the large majorityof cases there is nothing that indicates that the retinal detachment will occur before actually happens.
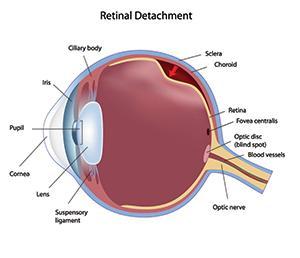 Retinal Detachment
Retinal Detachment
Physical symptoms rerceived by the patient might be:
• Flashes of light
• A shower of floaters
• A loss of peripheral visual field that the patient will not notice most of the times until the central vision has been affected
Without rapid surgical inovention preferably between 8 and 15 days the retina can become retracted because pigment cells will start to form membrans over the surface of the retina.
When the retina is retracted, surgery becomes much more complicated and the chances of healing are severely diminished.
Surgical treatment of Retinal Detachment
The first goal of surgical treatment is to stop the fluid from passing through the tear by plagging it.
The pumping done by the pigment epithelium allows the retina to be re-attached.
To do this the surgeon first needs to find all the tears or holes, no matter how small, in order to induce in an inflammatory reactionon the edges of the holes or tears by cryopexy or laser.
This reaction will act as a glue when the tear will be pushed against the pigment epithelium.
This can be done in a several ways. The doctor can re-shape the sclera pushing against the tear by doing a sclera buckle. Using an explants suture to the sclera he can do an internal tamponade by pushing the retina against the pigment epithelium and then injecting a bubble of gass into the eye.
This bubble will then be absorbed naturally. For complicated cases a silicone bubble is sometimes used instead, there must later be removed.

